 The flu vaccine is one of the mainstays of winter preparedness as flu viruses normally start circulating more over the winter months.
The flu vaccine is one of the mainstays of winter preparedness as flu viruses normally start circulating more over the winter months.
The vaccine is offered mainly to three groups of people. Firstly those at highest risk such as the elderly, those with long term conditions and pregnant women, who are most likely to be ill with flu and need hospital treatment. Secondly it is offered to healthy children using a nasal spray to provide direct protection to them and to interrupt spread in the community. Thirdly it is offered to those such as front line health and social care staff who are most likely to spread infection to those who are vulnerable .
The reality is that while most of the latter group will not be significantly affected themselves, they can and do spread it to those around them.
Why is it then that health care staff remain reluctant to get the vaccine?
The uptake of the vaccine varies considerably between different organisations but overall remains around 50% of those eligible actually get it.
As part of the Chief Nurse Directorate's Week of Action (#ProtectAoH) I’m going to look in turn at some of the reasons people use for not having the jab and make the case why they should have it.
The vaccine is not very effective
There are many different strains of flu virus and the makeup of the virus changes year on year. Each year the vaccine is made up with between 3 and 4 strains of flu virus, depending on the type of vaccine. These strains are determined annually after careful mapping of the circulating flu strains by the World Health Organization. The effectiveness varies year on year depending on how well the viruses are matched to those actually circulating.
So while it is true that the flu vaccine is not as effective in comparison to other vaccines there is good evidence that immunisation reduces the incidence of severe disease and hospitalizations in those most at risk[i].
I keep myself fit and well and never get ill
Younger fitter individuals are statistically less likely to be seriously ill with the flu. Even if they do get the infection, flu is a self limiting illness with symptoms lasting between 2 and 7 days. However, it is very infectious and easily transmissible.
Those infected, even if they are not symptomatic themselves, can spread the virus to vulnerable patients, which could result in them becoming seriously ill.
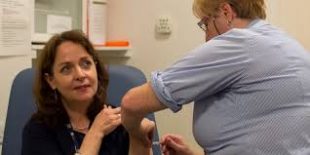
I always get ill after having the vaccine
As with having any vaccine, sometimes the short lived side effects from a vaccine can mimic flu. This is the result of the immune response, with symptoms such as a slight temperature and muscle aches. These symptoms are normal and generally very mild, the vaccine cannot cause someone to have the flu. The viruses in the vaccine cannot cause infection. The vaccine is rigorously tested prior to release.
There are always other circulating viruses that can cause flu-like symptoms which if they happen shortly after receiving the flu job, are often wrongly ascribed to being caused by the flu vaccine.
It is difficult to get the vaccine where I work
It is the responsibility of the employer to make the vaccine available to those likely to be in contact with vulnerable patients. However, there is also a professional responsibility to make sure we protect patients and therefore a need to ask for and demand the vaccine. Contact your occupational health department or line manager to find out how you can get vaccinated.
It is important to remember that it takes 10 – 14 days to develop immunity following vaccination, so it is important to get vaccinated as soon as possible before the flu season really starts.
If you haven’t already done so use this week of action ( https://vivbennett.blog.gov.uk/ ) to go and get the vaccine and, prepare for the winter ahead. Protect yourself and protect your patients.
Where can I find more information about the flu vaccine and healthcare workers?
There is excellent information in the NHS Employers flu fighter website here: http://www.nhsemployers.org/campaigns/flu-fighter
[i] Green Book (on Line) Influenza chapter 19 https://www.gov.uk/government/uploads/system/uploads/attachment_data/file/456568/2904394_Green_Book_Chapter_19_v10_0.pdf
Helen Donovan, Professional Lead for Public Health, Royal College of Nursing
